OpenPalp — Your Personal Heart Rhythm Programme
If your heart has been worrying you, you are not alone — and you do not have to keep wondering.
Dr Mahmood Ahmad — MRCP(UK), GMC verified — 40–44 The Broadway, Wimbledon
30 days of monitoring. 6 weeks of understanding.
A structured programme combining clinic assessment, 30 days of KardiaMobile ECG monitoring, and a guided lifestyle programme. Friday evenings in Wimbledon — no time off work.
You are not alone
Many palpitations are distressing but not dangerous
Palpitations are one of the most common reasons people visit a cardiologist. The sensation of your heart skipping a beat, fluttering in your chest, or suddenly racing can be alarming — but in the majority of people with no underlying heart disease, palpitations are a benign nuisance rather than a warning sign.
Most people find that their palpitations come and go unpredictably. This uncertainty is itself distressing. The OpenPalp programme is designed to give you answers: a clear record of what your heart is doing, an understanding of your personal triggers, and a structured plan to reduce the frequency and impact of symptoms.
Common triggers include:
- Caffeine
- Poor sleep
- Stress and anxiety
- Alcohol
- Dehydration
- Hormonal changes
You will find your personal triggers through this programme.
Every component of this programme is supported by published evidence, including a Cochrane review of 20 randomised trials (exercise), an NEJM randomised trial (alcohol reduction), and safety data from over 81,000 participants (omega-3 warning).
The attention loop
Why palpitations feel worse the more you notice them
The more you monitor your heartbeat, the more you find it — until you learn not to look.
Your journey
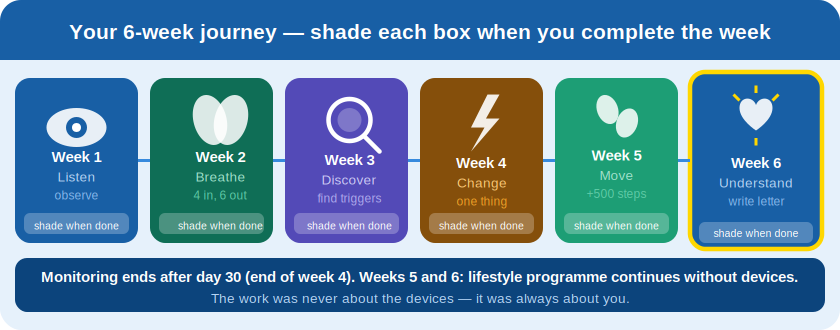
30 days of monitoring. 6 weeks of change.
Two things happen at once: your monitoring runs for 30 days, your lifestyle programme runs for 6 weeks.
How it works
Four simple steps
- Book your £60 clinic appointment online
- Attend your Friday evening appointment — Dr Ahmad assesses your symptoms and confirms suitability
- If suitable, pay £70 for the monitoring & programme — receive your KardiaMobile 6L and OpenPalp booklet on the same visit
- Start your 30-day monitoring and 6-week programme — with support throughout
Why not wait?
NHS cardiology wait vs this pathway
NHS Cardiology Referral
12–18 weeks
Typical wait for a routine NHS cardiology outpatient appointment
This Pathway
This Friday
Clinic assessment available Friday evenings in Wimbledon SW19
A typical private cardiology initial consultation costs £200–£350. Our full pathway — including monitoring and a six-week programme — costs £130 total.
Your clinician
Dr Mahmood Ahmad
Specialist in Cardiology (SAS grade — a senior NHS specialist role) · MRCP(UK) · GMC 6071047

All care within the OpenPalp pathway is delivered by Dr Ahmad. He works independently on the consultant cardiology rota at the Royal Free Hospital and Barnet Hospital, and brings extensive experience in managing common cardiac conditions in private practice. He is fully GMC-registered and fully insured for independent private practice.
Transparency
Dr Ahmad works independently on the consultant cardiology rota at the Royal Free Hospital and Barnet Hospital. He is fully GMC-registered (with licence to practise), holds MRCP(UK), and is fully insured for independent private practice. His career pathway to Specialist grade was different from the traditional NHS consultant training programme — he does not hold a CCT, a credential specific to that training route. His clinical role and right to independent practice are not dependent on holding a CCT.
Pricing
Transparent and affordable
Two clear costs. No hidden fees.
Clinic Appointment
Face-to-face assessment with a specialist
£60
one-off payment
- Face-to-face assessment
- Symptom and trigger review
- Risk factor assessment
- ECG if clinically indicated
- Suitability confirmation
- Clear explanation and next steps
Monitoring & Programme
Device, booklet, guided programme, and review
£70
one-off payment
- KardiaMobile 6L (30 days of event recording)
- OpenPalp printed booklet & digital booklet
- 6-week guided programme
- Review of all recordings
- Results appointment and findings letter
- 15-minute in-person results appointment at day 30
- Review your Kardia recordings and booklet together with Dr Ahmad
Full pathway total
£130
If the KardiaMobile is lost or damaged: replacement cost £70. The clinic appointment is standalone — there is no obligation to proceed to the monitoring programme.
Ready to take the first step?
Your £60 clinic appointment is standalone — no commitment to the full programme.
40-44 The Broadway, Wimbledon, London SW19 1RQ · Friday evenings 17:00–20:00
Free cancellation up to 48 hours before your appointment. Late cancellations and no-shows may be charged in full.
OpenPalp — The Programme
THE PROGRAMME
Six weeks of structured support
Each week has one focus. Build on the one before.
Every component is supported by published evidence — including three high-quality landmark trials (Cochrane, NEJM, Circulation).
Listen
Start your Kardia. Begin your diary. Simply observe. Every entry is a clue. Monitoring runs this week and for 30 days total. Structured self-monitoring is supported by moderate-quality evidence from an umbrella review of 39 systematic reviews.
Breathe
Five minutes of slow breathing, twice a day. 4 seconds in, 6 seconds out. In a meta-analysis of 31 studies, this changed heart rhythm within the same session — not after weeks. Within minutes.
Discover
Look back at your diary. Find your two personal triggers. In studies of people with palpitations, 71% found stress, 62% caffeine, 58% sleep disruption. You are part of a very human pattern. This week, experiment with caffeine — and consider your alcohol intake. A landmark NEJM trial found that reducing alcohol cut AF recurrence by 45%.
Change
Act on your top trigger. One change. Seven days. The same heart responds differently to a different life. This is the week you test that. Sleep quality matters — the UK Biobank study of 403,000 people found insomnia increases AF risk by 30%. And if weight is relevant, the REVERSE-AF study showed 88% AF reversal with 10% or more weight loss.
Move
Monitoring has ended. Return your Kardia at your results appointment. Your programme continues. Set your step baseline and add 500 per day. Exercise has the strongest lifestyle evidence of all — a Cochrane review of 20 randomised trials found a 30% reduction in AF recurrence (RR 0.70). Movement is medicine.
Understand
Final week. Review your progress, practise vagal techniques (the REVERT trial showed the modified Valsalva achieves 43% SVT reversion vs 17% standard), and consolidate everything you have learned. Fill in your progress tracker. Write your letter. See how far you have come.
Day 30
Your results appointment
At the end of your 30 days, you return for a 15-minute appointment with Dr Ahmad. Bring your Kardia device and your completed booklet. Together, you will review every recording in the app, look at your diary entries, and discuss what your heart has been telling you. You will receive a clear explanation of findings and a management plan. With your consent, a summary is sent to your GP within 5 working days.
When you feel palpitations
Most episodes pass within a few minutes. Here is what to do — in order.
If you feel faint, develop chest pain, or experience a sustained fast heart rate that does not settle after 15–20 minutes, stop and call 999 immediately. Do not attempt the steps below.
Stay calm
Anxiety amplifies palpitations. Take one slow breath and remind yourself: most palpitations are not dangerous. You are not in danger.
Sit or lie down
Reduce demand on your heart. Do not continue strenuous activity until the episode has fully passed.
Breathe slowly
4 seconds in. 6 seconds out. Repeat five times. This activates your vagus nerve and can slow or settle the heart.
Try a vagal technique
If you feel safe to do so: bear down gently as if straining (Valsalva), or splash cold water on your face. Only if you feel well enough.
Record on Kardia
As quickly as possible. Even if symptoms are settling — record anyway. A trace during or just after an episode is highly informative.
Write in your diary
Time, duration, severity, what you were doing, what helped. The pattern across 30 days is where the answers live.
Important note on vagal techniques
Not suitable if you have known eye disease or significant heart valve problems. Do not press on your neck (carotid massage). If symptoms worsen during any technique, stop immediately. If you feel very unwell or develop chest pain, do not attempt them — call 999. Always sit or lie down first.
Your daily practice
Small consistent actions change the nervous system more than anything else. You do not need to be perfect. You need to be regular.
Every morning
- Check your HRV if your watch tracks it — note the number in your diary
- Take one resting Kardia recording — before getting up
- Five minutes of 4-6 breathing. In for 4, out for 6.
- Fill in your diary for yesterday
Every evening
- Five minutes of 4-6 breathing
- Note one thing that helped your heart today
- Rate your heart anxiety today (1–10) in your diary
- Note your steps for the day
If anything concerns you during the programme, email drmahmoodclinic@pm.me — Dr Ahmad typically responds within 4 hours during working days.
If your symptoms change during the programme
If your palpitations become more frequent, more severe, or different from usual, or if you develop new symptoms such as fainting, chest pain, or breathlessness, contact the clinic by email or call your GP. If urgent, call 111 or 999.
Understanding HRV — your nervous system score
Heart rate variability (HRV) is the variation between heartbeats. A higher number means your nervous system is calm and adaptable. A lower number means it is under strain.
You do not need to analyse it. Just watch the trend. Most people see their HRV rise over six weeks as their nervous system settles.
Your two lifestyle experiments
Experiment 1 — The caffeine test (week 3)
Replace your first coffee with hot water and lemon for 7 days. Note your palpitations in the diary each day. Week 4: reintroduce caffeine. Compare. If palpitations increase, caffeine is your trigger.
Experiment 2 — The sleep anchor (week 4)
Set one fixed wake time. Keep it for 7 days — even weekends. Stop caffeine after 2pm. Note sleep quality in your diary each morning. This single change often reduces palpitations within days.
OpenPalp — Your Device
YOUR DEVICE
Your device
Kardia — your handheld ECG (30 days)
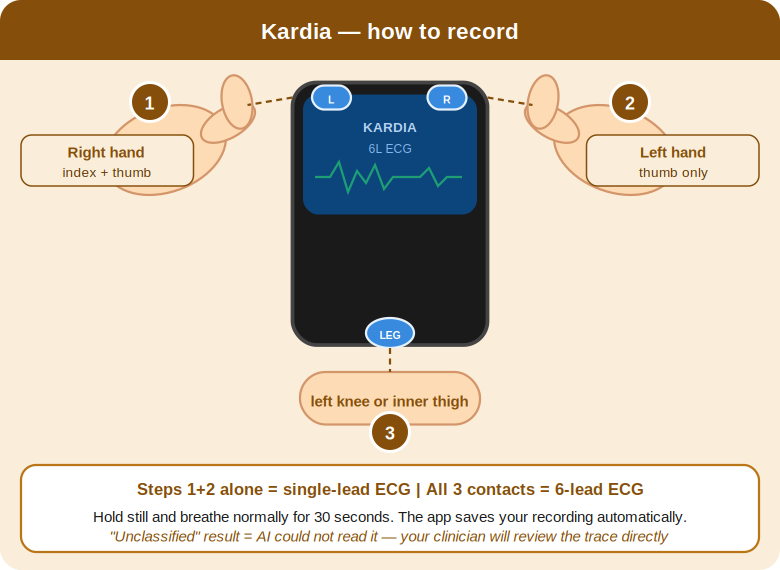
The Kardia is yours to use whenever you feel something. Think of it as your heart’s voice recorder — activated by you, at the moment that matters.
Setting up
- Download the free Kardia app (App Store or Google Play)
- Open app, tap ‘Add a device’, follow pairing steps
- No paid subscription needed — free tier stores all ECGs
How to record
- Left thumb on bottom electrode — right index finger and thumb on top two
- For a fuller picture, rest back of device on left knee
- Hold still, breathe gently, stay for 30 seconds
- App saves and analyses recording automatically
When to record
Record whenever you feel symptoms — as quickly as you can. Also take one morning resting recording each day, before getting up. This builds a baseline picture. Note the time of each recording in your diary.
At your results appointment
Open the Kardia app and show Dr Ahmad your full recording history. You review them together.
If the app says ‘Unclassified’ — that means the AI could not read it. Your clinician will review the trace directly.
What if your Kardia shows a concerning result?
If the app displays “Possible Atrial Fibrillation” or another concerning result, do not panic. Record the ECG and note the time in your diary. Email drmahmoodclinic@pm.me with the date and time of the recording — Dr Ahmad will review it promptly. If you also feel unwell, faint, or have chest pain, call 999.
Device loan
The KardiaMobile 6L is loaned for the duration of the programme. You return it at your results appointment.
If the Kardia is lost or damaged beyond reasonable wear: replacement cost £70.
OpenPalp — Suitability
Suitability
Is this pathway right for you?
This service is designed for selected low-risk patients. Please review the criteria below carefully.
Most people with palpitations will not have these features. If you are unsure about any item below, attend the clinic appointment — Dr Ahmad will assess you and advise.
This pathway is designed for you if
- You are aged 18 or over
- You have intermittent palpitations — an awareness of your heartbeat
- Episodes are brief, lasting seconds to minutes
- You feel generally well between episodes
- You have no known significant heart disease
- Symptoms include missed beats, skipped beats, or occasional rapid episodes that settle on their own
- Symptoms are associated with caffeine, stress, poor sleep, or anxiety
This pathway is not suitable if
- You have fainted or nearly fainted
- You have chest pain that may be cardiac in origin
- You have severe or unexplained breathlessness
- Your heart races for more than 20–30 minutes without settling
- You have known structural heart disease or heart failure
- You have a known significant arrhythmia requiring management
- You have had cardiac surgery or complex congenital heart disease
- Your symptoms are clearly triggered by exertion
- You have a strong family history of sudden cardiac death
- You have an abnormal baseline ECG that needs investigation
- You have a pacemaker or ICD in situ
Borderline — clinical judgement required
- More frequent or prolonged episodes
- Mild exertional symptoms without other red flags
- Unclear history
- Previous investigations but persistent symptoms
These patients may enter the pathway after clinician review, or be referred onward directly.
What if I attend and turn out not to be suitable?
If Dr Ahmad determines during your appointment that you need a different pathway, you will be advised clearly on the day. You will still receive a clinical opinion, a resting ECG if indicated, and a written summary for your GP. You will not be left without a plan.
What if monitoring finds something significant?
If monitoring reveals atrial fibrillation, SVT, significant pauses, or a high ectopy burden, you will be referred promptly to NHS cardiology. You will not be left without a plan.
If examination findings suggest structural heart disease — such as a murmur, abnormal ECG, or signs of ventricular hypertrophy — you will be referred for echocardiography and specialist assessment. Echocardiography is not performed at this clinic, but referral is arranged promptly when indicated.
If your thyroid function has not been checked recently, Dr Ahmad may recommend a blood test through your GP — thyroid disorders are a common and treatable cause of palpitations.
Supplement safety check
At your appointment, we will review any supplements you are taking — including omega-3 fish oil, which recent high-quality evidence (7 RCTs, 81,210 participants) suggests may increase arrhythmia risk by 25%. If you take fish oil supplements, please mention this to Dr Ahmad.
OpenPalp — The Evidence
The Evidence
These are not theories
They are findings from real studies involving real people — people whose hearts changed when they changed how they lived.
View Interactive Evidence Dashboard →Exercise — the strongest lifestyle evidence
(Buckley et al., Cochrane 2024 — 20 RCTs)
A Cochrane systematic review — the gold standard of evidence synthesis — found that exercise-based cardiac rehabilitation reduces AF recurrence by 30% (RR 0.70, 95% CI 0.56–0.88). This is the strongest lifestyle evidence in the entire programme. Separately, a meta-analysis of 1.46 million people confirmed that guideline-level physical activity protects against AF onset.
Regular moderate exercise is not just good for the heart. It is one of the most effective interventions in all of cardiology for reducing arrhythmia burden.
Buckley BJR, et al. Cochrane Database Syst Rev. 2024. • Mishima RS, et al. Heart Rhythm. 2021;18(7):1203-1213.
Alcohol reduction — the only lifestyle RCT in the NEJM
(Voskoboinik et al., New England Journal of Medicine, 2020 — RCT, n=140)
In the first randomised trial of alcohol abstinence for AF, patients who stopped drinking reduced their AF recurrence by 45% (HR 0.55, 95% CI 0.36–0.84). AF burden fell from 1.2% to 0.5% of total time. Even moderate regular drinking (10+ drinks per week) has measurable cardiac effects.
This was not an observational study. This was a controlled trial, published in the most prestigious medical journal in the world, showing that one lifestyle change — reducing alcohol — cut AF recurrence nearly in half.
Voskoboinik A, et al. N Engl J Med. 2020;382:20-28.
Omega-3 fish oil supplements — increased AF risk
(Gencer et al., Circulation, 2021 — 7 RCTs, n=81,210)
Counter-intuitively, omega-3 fish oil supplements increase the risk of atrial fibrillation by 25% (HR 1.25). At doses above 1g per day, the risk rises to 49% (HR 1.49). This is a large, high-quality meta-analysis of randomised controlled trials with a clear dose-response relationship. Eating fish as part of your diet does not carry this risk.
If you are taking omega-3 supplements to help your heart, the evidence suggests they may be making your rhythm worse, not better. Mention all supplements at your appointment.
Gencer B, et al. Circulation. 2021;144:1981-1990.
The breathing story
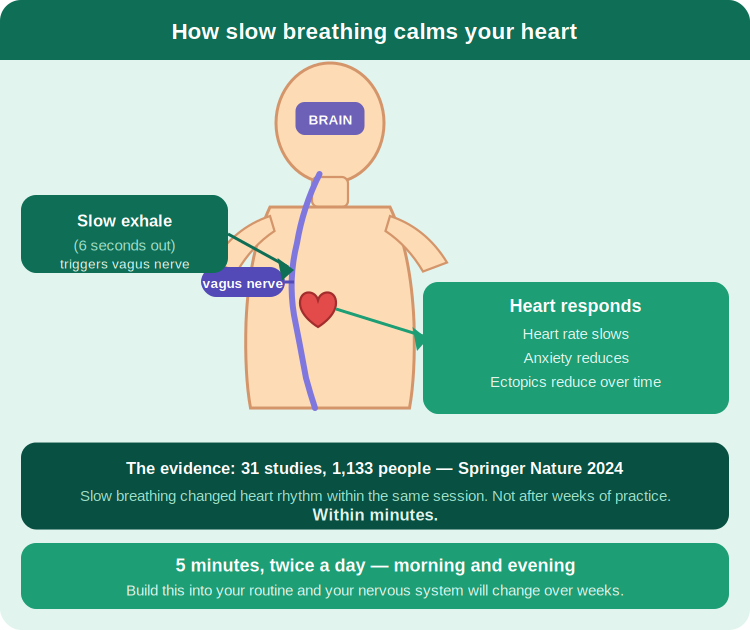
(Springer Nature, 2024 — meta-analysis of 31 studies, n=1,133)
Researchers gathered 31 studies involving 1,133 people. Some were anxious. Some had high blood pressure. Some had palpitations. All of them were asked to do one thing: slow their breathing to fewer than 10 breaths per minute for five minutes.
In every group, heart rate variability improved. Not after weeks of practice. Within the same session. Within minutes. The vagus nerve — the body’s main brake on the heart — responded to the exhale. Longer out than in. The heart slowed. The anxiety eased.
Five minutes, twice a day — morning and evening. Build this into your routine and your nervous system will change over weeks.
Laborde S, et al. Sci Rep. 2024;14:2881. doi:10.1038/s41598-024-53389-8
The sleep story

Miner et al., SLEEP, 2016 — a study of hospital alarm noise found that on quieter nights, PVCs fell by 33%. They stayed lower the following day.
A 2021 study in JACC followed 403,187 UK Biobank participants and found a 29% lower risk of atrial fibrillation in those with healthy sleep patterns.
Your sleep is not separate from your heart rhythm. It is part of it.
Kwon Y, et al. J Am Coll Cardiol. 2021;78(21):2029-2041.
Miner SEJ, et al. SLEEP. 2016;39(Suppl):A297.
Weight, movement, and the heart
(PubMed, 2015 — 22,516 adults, 14-year follow-up)
Over 14 years, researchers followed 22,516 apparently healthy men and women attending health screenings. They measured weight, activity, and heart rhythm. Obese patients were 33% more likely to have ectopic ventricular beats. Every additional unit of BMI added 4% more risk.
In absolute terms, these risks are small for most people. These figures describe population trends, not individual predictions.
Separately, large observational studies have found that regular moderate physical activity is associated with a significantly lower risk of atrial fibrillation.
Not because of a disease — because of how they were living. The heart that moves less, fires irregularly more.
Ataklte F, et al. BMC Cardiovasc Disord. 2015;15:176.
The most important story in modern cardiology
This story has a reassuring ending — and it changed how we think about the heart forever.
In 1989, doctors ran a trial. They had a drug that successfully suppressed extra heartbeats after heart attack. The logic seemed obvious: fewer extra beats, less risk of sudden death. The trial was stopped early. Patients taking the drug were dying at three times the rate of those who took nothing.
(CAST Trial, 1989)
The lesson was profound and it changed cardiology permanently: extra heartbeats are a signal, not always the problem. Silencing them without understanding them can be worse than leaving them alone. Understanding them — as you are doing — is often more important than trying to suppress every extra beat.
The Cardiac Arrhythmia Suppression Trial (CAST) Investigators. N Engl J Med. 1989;321:406-412.
Lifestyle factors: alcohol and weight
A 2020 randomised trial published in the New England Journal of Medicine found that alcohol abstinence reduced AF recurrence by 45% compared to continued moderate drinking. The effect was dose-dependent: even light drinking was associated with increased recurrence.
The REVERSE-AF study demonstrated that sustained weight loss has a profound impact on AF burden. Patients who lost 10% or more of their body weight achieved an 88% rate of AF reversal — compared to just 26% in those who lost less than 3%.
Important: Omega-3 fish oil supplements may increase the risk of atrial fibrillation. A meta-analysis of 81,210 participants found a 25% increased AF risk, with higher doses (above 1g/day) carrying a 49% increased risk. If you take omega-3 supplements, mention this at your appointment.
Voskoboinik A, et al. N Engl J Med. 2020;382:20-28. • Pathak RK, et al. J Am Coll Cardiol. 2015;65(21):2159-2169. • Gencer B, et al. Circulation. 2021;144:1981-1990.
OpenPalp — Frequently Asked Questions
Questions
Frequently asked questions
You will be seen in a private consultation room. The appointment lasts about 30 minutes. Dr Ahmad will review your symptoms, medical history, and triggers in detail. You may have an ECG taken. You will receive a clear explanation of findings on the day, and a written summary is sent to your GP (with your consent) within 5 working days. The clinic is at 40–44 The Broadway, Wimbledon SW19 1RQ.
The KardiaMobile 6L is a small handheld device that records a medical-grade six-lead ECG in 30 seconds. You use it whenever you feel symptoms, and once each morning at rest. It is loaned for the 30-day monitoring period. At your results appointment, you open the app and review the recordings together with Dr Ahmad.
No. Your £60 clinic appointment is completely standalone. After your appointment, you can decide whether to continue with monitoring and the six-week improvement programme (£70). There is no obligation and no pressure.
A normal resting ECG is reassuring, but it only captures a few seconds of your heart rhythm. Many palpitations are intermittent, which is why this pathway includes monitoring over 30 days — to catch what a single ECG often misses.
If monitoring identifies a significant rhythm abnormality — such as SVT, atrial fibrillation, significant pauses, or high ectopy burden — you will be referred to an appropriate NHS specialist. We provide documented findings and a clear summary to the receiving clinician.
If monitoring does not capture an abnormal rhythm, that itself is useful information. Combined with a normal clinical assessment, it provides meaningful reassurance. The improvement programme can still help reduce symptom frequency. If clinical concern persists, you will be referred onward.
The KardiaMobile 6L is loaned for the duration of the programme. You return it at your results appointment. There is no deposit or pre-authorisation. If the device is lost or damaged beyond reasonable wear, the replacement cost is £70.
No. Fainting (syncope) associated with palpitations is a red flag that requires urgent or specialist assessment. This pathway is for low-risk patients without syncope.
40–44 The Broadway, Wimbledon, London SW19 1RQ. Approximately five minutes from Wimbledon station. Appointments are available on Friday evenings, 17:00–20:00.
Because most low-risk palpitations are influenced by modifiable factors — caffeine, stress, sleep quality, activity levels, and how you respond to symptoms. Monitoring alone tells you what your heart is doing. The improvement programme aims to help you influence what it does next.
Yes. This pathway does not prevent or replace referral to a cardiologist. If significant findings emerge, or if symptoms persist beyond the pathway, referral is arranged. Patients may also choose to see a private cardiologist independently at any time.
While eating fish is part of a healthy diet, omega-3 fish oil supplements may actually increase the risk of atrial fibrillation. A meta-analysis of 81,210 people found a 25% increased risk with supplements, particularly at doses above 1g per day. If you currently take fish oil supplements, mention this at your appointment.
OpenPalp — Patient Feedback
Patient Feedback
What patients say
What the 6-week programme looks like in practice.
Week 1
“Recording my first Kardia trace felt empowering. For the first time, I could see what my heart was actually doing instead of just worrying about it.”
Week 3
“The caffeine experiment was a revelation. I had no idea my afternoon coffee was the trigger. Five days without it and the skipped beats almost stopped.”
Week 6
“My heart anxiety score dropped from 8 to 3. The breathing technique and understanding the attention loop changed everything.”
Illustrative examples based on typical programme outcomes. Individual results vary.
Completed the programme? We would love to hear about your experience.
Share Your FeedbackOpenPalp — For Clinicians
For Clinicians & Referrers
OpenPalp Pathway
Patients may self-refer. This page is for clinicians who wish to understand the pathway or discuss patient suitability.
Pathway focus
This pathway is designed for adults with low-risk palpitations who are otherwise well and have no high-risk features.
Inclusion criteria
- Intermittent palpitations (awareness of heartbeat)
- Brief episodes (seconds to minutes), settling spontaneously
- No loss of consciousness
- No known significant structural heart disease
- No prior high-risk arrhythmia diagnosis
- Generally well between episodes
Exclusion criteria
- Syncope or pre-syncope
- Chest pain suggestive of cardiac origin
- Severe or unexplained breathlessness
- Sustained tachycardia (>20–30 minutes)
- Known structural heart disease, heart failure, or significant arrhythmia
- Exertion-triggered symptoms
- Strong family history of sudden cardiac death
- Abnormal baseline ECG requiring investigation
- Pacemaker or ICD in situ
Monitoring protocol
- KardiaMobile 6L — 30 days of patient-activated event recording
Escalation thresholds
- SVT or significant supraventricular tachycardia
- Atrial fibrillation or flutter
- Significant pauses (>3 seconds)
- High ectopy burden (>10% of recorded beats)
- Symptoms remaining unexplained after completion of the pathway
- Persistent clinical concern
Six-week programme
- Week 1 — Listen
- Week 2 — Breathe
- Week 3 — Discover
- Week 4 — Change
- Week 5 — Move
- Week 6 — Understand
Governance
- This service is for selected low-risk patients only. Not a substitute for comprehensive cardiology care.
- Every patient assessed at initial appointment to confirm suitability.
- Clear referral thresholds defined. Significant findings are escalated.
- Not an emergency service. Does not replace urgent or hospital care.
- Monitoring recordings reviewed within clinic pathway. Complex findings escalated.
- Improvement programme is supportive and behavioural. Does not replace medical treatment.
- Unexplained symptoms after pathway completion are escalated.
Service delivery
All care is delivered by Dr Mahmood Ahmad, Specialist in Cardiology (SAS), MRCP(UK), GMC 6071047. Dr Ahmad practises independently on the consultant rota at the Royal Free Hospital and Barnet Hospital. He is fully GMC-registered and fully insured for independent private practice.
Transparency: Dr Ahmad reached his Specialist grade through a career pathway different from the traditional NHS consultant training programme. He does not hold a Certificate of Completion of Training (CCT) and is not on the GMC Specialist Register.
Communication
With patient consent, a written summary of findings, ECG results, and management plan is sent to the referring or registered GP within 5 working days. Red-flag ECG recordings are reviewed by Dr Ahmad within 24 hours and the patient is contacted directly.
Referral
Patients may self-refer. If you would like to refer a patient or discuss suitability, please contact drmahmoodclinic@pm.me.
For GPs: referring your patient
No formal referral is required — patients can self-refer online. However, if you would like to refer directly or discuss a patient's suitability, please email drmahmoodclinic@pm.me with a brief clinical summary.
After the programme, a written summary of findings is sent to the patient's GP (with consent), including any Kardia recordings of clinical significance.
Dr Mahmood Ahmad — Specialist in Cardiology (SAS grade), MRCP(UK), GMC 6071047. Royal Free Hospital and Barnet Hospital.